There are many potential health issues for people to look out for as they age, and hyperparathyroidism is one of them. In particular, women between the ages of 30 and 60 need to stay alert for signs of hyperparathyroidism. Before patients can understand what hyperparathyroidism symptoms to watch out for, it’s helpful to know what hyperparathyroidism is and what risk factors exist.
What is Hyperparathyroidism?
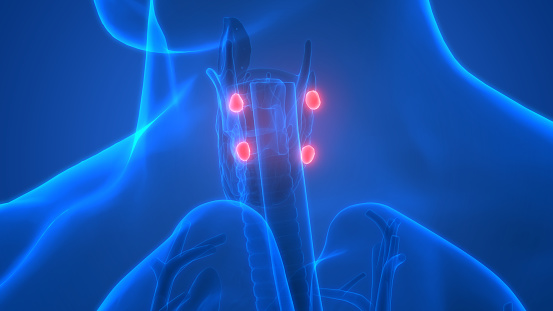
Hyperparathyroidism occurs when one of the four parathyroid glands in the neck becomes overactive. This causes the gland, or sometimes multiple glands, to produce too much parathyroid hormone. Parathyroid hormone (PTH) helps regulate calcium levels in the body. While calcium is most well-known for its role in keeping bones and teeth healthy, the mineral also helps muscles contract, regulates heart rhythms, supports nerve function, and facilitates proper blood clotting.
or sometimes multiple glands, to produce too much parathyroid hormone. Parathyroid hormone (PTH) helps regulate calcium levels in the body. While calcium is most well-known for its role in keeping bones and teeth healthy, the mineral also helps muscles contract, regulates heart rhythms, supports nerve function, and facilitates proper blood clotting.
To help prevent calcium levels in the bloodstream from dropping too low, parathyroid hormone releases calcium from the bones into the bloodstream, maximizes calcium absorption from food, and helps kidneys retain calcium and return it to the bloodstream rather than flush it out through urine.
If the parathyroid glands are malfunctioning and making too much PTH, this means that too much calcium is released from the bones. There are three types of hyperparathyroidism.
- Primary HPT: A noncancerous tumor (adenoma) grows on one or more of the four rice-sized parathyroid glands in the neck, causing overproduction of PTH.
- Secondary HPT: A disease outside of the parathyroid glands, such as kidney disease or vitamin D deficiency, causes all four parathyroid glands to become enlarged.
- Tertiary HPT: This type of HPT occurs when secondary HPT persists even after a kidney transplant or dialysis.
Left untreated, hyperparathyroidism can result in several complications, including osteoporosis and kidney stones.
(Photo/ Unsplash)
Complications of Untreated Hyperparathyroidism
Calcium is essential in helping to build healthy bones. However, overproduction of PTH means that calcium is consistently being drawn out of the bones. This weakens them and can lead to fragility, fractures and osteoporosis.
Excessive calcium in the blood can also cause the urine to carry too much calcium, resulting in kidney stones—small, hard calcium deposits in your kidneys that must pass through the urinary tract to exit the body. This often results in intense pain. If a stone is too large to fit through the urinary tract, medical intervention may be necessary to break up the stone so it can pass through the body.
While these are the more common risks of untreated hyperparathyroidism, other complications can arise. Hyperparathyroidism has been linked to heart disease. And while primary hyperparathyroidism isn’t common for women in their childbearing years, untreated primary hyperparathyroidism in a mother can cause dangerously low calcium levels in newborns. Understanding this condition’s causes and risk factors can help a person assess whether they might be at risk of developing the disease.

Hyperparathyroidism Risk Factors and Causes
Women in general, and particularly women around the ages of 50 to 60, are the most at risk of developing hyperparathyroidism. While hyperparathyroidism can develop in menstruating women, it’s less common. Men can get hyperparathyroidism as well.
Anyone who has had radiation therapy or other cancer treatments targeted toward the neck area is at risk of developing hyperparathyroidism, too, as are those who take medications that may alter calcium levels. If hyperparathyroidism runs in a person’s family, that person may be more likely to develop the condition due to heredity.
As with the risk factors for hyperparathyroidism, the causes of HPT can vary. In primary hyperparathyroidism, the causes can include:
- Parathyroid adenomas, which are benign tumors of the parathyroid gland
- Hyperplasia, or the enlargement of all four parathyroid glands
- Cancerous tumors on the parathyroid glands, which tend to be rare
Secondary hyperparathyroidism is most often caused by severe calcium deficiency, severe vitamin D deficiency, or chronic kidney failure. Tertiary hyperparathyroidism occurs after long-term secondary HPT, particularly if the HPT fails to improve in a kidney disease patient following kidney disease treatment.
(Photo/ Unsplash)
8 Most Common Hyperparathyroidism Symptoms
Hyperparathyroidism is notorious for its nonspecific symptoms. People suffering from the condition may complain of depression and joint pain only to have a provider shrug the symptoms off as stress or aging. However, blood tests to measure PTH and calcium should be conducted if a person has one or more of the symptoms below.
The 8 most common symptoms of hyperparathyroidism are
- Kidney stones
- Abdominal pain
- Bone and joint pain
- Increased need to urinate
- Becoming tired too easily
- Feeling weak
- Depression
- Nausea and vomiting
If you have any risk factors for hyperparathyroidism and are experiencing these symptoms, or even if you don’t have a known risk factor for HPT, consulting with a parathyroid specialist is an important step toward finding treatment.

Diagnosing and Treating Hyperparathyroidism
Hyperparathyroidism is diagnosed using blood tests that measure PTH and calcium levels in the blood. Computed tomography (CT) scans, ultrasounds, X-rays, and sestamibi scans can also help diagnose hyperparathyroidism. In addition, these scans help a skilled parathyroid surgeon figure out where the problem gland is and map out a treatment plan.
Treatment can vary based on whether a patient has primary, secondary, or tertiary HPT. Primary HPT requires surgery to remove the parathyroid gland that’s causing a problem. Because secondary HPT is often caused by kidney issues, kidney disease treatment, medications, and calcium and vitamin D supplements are common treatments. For tertiary HPT, medication and surgery are both options.
A skilled parathyroid surgeon can perform a minimally invasive parathyroidectomy to treat hyperparathyroidism. This surgery doesn’t require general anesthesia or an extended hospital stay. In addition, the incision is small, and a good surgeon will take care to help the incision blend in with the neck’s natural creases. Symptoms of hyperparathyroidism should begin to decrease in the days, weeks, and months after parathyroidectomy.
(Photo/ Unsplash)
Schedule a Consultation
The CENTER for Advanced Parathyroid Surgery is helmed by a board-certified head and neck surgeon Babak Larian, MD, FACS. Dr. Larian utilizes leading-edge techniques, including intraoperative PTH testing and in-surgery pathology testing, to help ensure the success of every parathyroid surgery he performs. Dr. Larian values each patient who walks through his door, and he will work with a patient to develop a treatment plan that considers the patient’s symptoms, concerns, and questions.
If you are concerned, you may be dealing with one or more of the common hyperparathyroidism symptoms, schedule an appointment with a trusted surgeon or give Dr. Larian a call.
Sources:
Source: Free Guest Posting Articles from ArticlesFactory.com